TCM is an inheritance of Chinese culture. It has been used for the prevention and cure of diseases throughout the history of China. Over thousands of years, Chinese herbal medicine has played a crucial role in the healthcare of the Chinese people.
In the past few decades, the obvious side effects of chemical medicines, the expansion of new diseases in the world, the change of healthcare systems, and the trend toward natural approaches and restoring natural medicine have welcomed a different approach that could provide many opportunities for TCM. However, Chinese herbal medicine has its own governing theories of TCM practice and as a result cannot be covered by the framework of bio-medicine. The core of TCM rests on the restoration of the balance of the entire body. Herbal medicine is intended to help restore the normal functional states of each organ, to expedite recovery of the meridian system, and to promote the self-restoration of the body.
The modernization of Chinese herbal medicine in a way which retains basic theories and proven features is crucial, as these can be easily lost when it is following or resembling the approach of bio-medicine. As the fundamental theories, the Yin and Yang theory and the Five Elements theory are applicable to both Chinese herbal medicine and TCM. Nowadays, many often misunderstand or ignore the Yin and Yang theory. In fact, the Yin and Yang theory reflects not only the concept of opposition and unification, but also the primary and secondary relationships between the two sides; Yang does not equate to Yin, but rather commands Yin, and Yin is subordinate to Yang; more concisely, the whole determines the part. In life science, the Yin and Yang theory implies that the natural environment determines the individuals who live in it. It also implies that the inner environment reflects the “whole will” which determines the individual cells. Therefore, the TCM characteristics for curing diseases are the adjustments of the inner environment, which help achieve a balance between the human body and its surroundings.
Herbal medicine is based on a set of systematic theories. The theory of “Qi monism” is the foundation of all other TCM theories; it attributes everything in nature to a different combination of Qi, directly influencing herbal medicine selection. Essentially, human beings are linked to all substances of nature, and the human body can convert anything in nature into a useful element. Most Chinese herbs are derived from plants that are evolutionally similar to human beings, not only in their chemical composition but also in their unification with water. Hence, natural herbal medicines are easily absorbed by the human body, even as supplemental nutrition.
The meridian system in the human body communicates the information through the periodical dispersion and combination of water embedded around the inorganic ions. In bio-medicine, chemical drugs can be transmitted everywhere in the body through blood circulation. They change the threshold of information transformation, hence changing the function of the local tissue. This change restrains the regular function of the tissue. However, Chinese herbal medicine is different. Being composed of plant products, Chinese herbal medicine has similar components to living entities, such as proteins, amino acids, alkaloids, and tannin. These materials have minimum side effects yet favorable treatment effects due to their similarity to human body cells and their synergetic properties. They help restore the energy equilibrium and enhance the tissue function in the human body. Therefore, the herbs have an automatic and bi-directional selectivity, along with functions to adjust the balance of the body systems.
Herbal prescriptions incorporate many principles established by Zhang Zhongjing, known as “the sage of TCM,” who lived 2000 years ago. He wrote the book Treatise on Cold Diseases, and established the fundamentals of Chinese herbal medicine, such as “to clearly recognize the Yin–Yang situation, and support Yang as the first consideration.”
Collection and Preparation of Herbs
Collection of Herbs
The amounts of active ingredients in medicinal parts of animals or plants vary from time to time during their growth, which directly influences their qualities and curative effects. Therefore, it is important to time the collection of ingredients well, when the contents of active ingredients in medicinal parts reach the peak level. The time for collecting different medicinal parts of plants can be summed up as follows:
(1)Whole plants, stems, and leaves are mostly collected when the plants are in full-bloom or in early blossom, either by cutting off their parts above the ground or by pulling up whole plants with their roots. Seedlings or withered leaves are also used in some herbs, such as Oriental wormwood (Yin Chen,  ) and mulberry leaf (Sang Ye,
) and mulberry leaf (Sang Ye,  ).
).
(2)Flowers are generally collected in bud or in early blossom, to avoid dispersion of their fragrance and shedding of their petals. Pollen is collected in full blossom.
(3)Fruits and seeds are mostly collected when they are ripe. Only a few of the fruits are collected when they are unripe, such as black plum (Wu Mei,  ) green tangerine orange peel (Qing Pi,
) green tangerine orange peel (Qing Pi,  ), and unripe bitter orange (Zhi Shi,
), and unripe bitter orange (Zhi Shi, 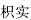 ). Some kinds of seeds easily shed when they are fully ripened.
). Some kinds of seeds easily shed when they are fully ripened.
(4)Roots and rhizomes are mostly collected in early spring, when plants have not sprouted, or in late autumn, when the stem and leaves start withering. At that time, nutrients and active ingredients stored in roots and rhizomes are at their peak concentration. A small number of herbs can be collected in summer, such as Pinellia tuber (Ban Xia) and Corydalis tuber (Yan Hu Suo, 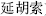 ).
).
(5)Bark should be collected in spring and summer, when it is thick with adequate fluid and nutrients and is easily stripped off. Root-bark should be collected in autumn, such as moutan root-bark (Mu Dan Pi, 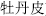 ) and wolfberry root-bark (Di Gu Pi,
) and wolfberry root-bark (Di Gu Pi, 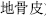 ).
).
Preparation of Herbs
Herbs should be processed before using them or making them into various forms. However, most Chinese herbs used are unprepared and clean, besides general handling, and quite a few should be specifically processed to meet demands for their clinical use. Strict preparation techniques were developed in a long history of practice of traditional Chinese pharmaceutical technology.
(1) Aims of preparation
High effect, low toxicity, and convenience for use are the main aims of preparing Chinese herbs.
(a)To enhance curative effects
Examples: Corydalis tuber (Yan Hu Suo, 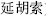 ) can obviously strengthen its analgesic effect by stir-baking with vinegar; Ephedra (Ma Huang,
) can obviously strengthen its analgesic effect by stir-baking with vinegar; Ephedra (Ma Huang, 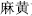 ) can strengthen the effects of alleviating cough, and relieving asthma by stir-baking with honey; and Eucommia bark (Du Zhong,
) can strengthen the effects of alleviating cough, and relieving asthma by stir-baking with honey; and Eucommia bark (Du Zhong, 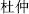 ) can strengthen the effects of calming the liver and reducing blood pressure by stir-baking with salt.
) can strengthen the effects of calming the liver and reducing blood pressure by stir-baking with salt.
(b)To reduce toxic effects
Some extremely toxic herbs should not be used orally without preparation for reducing their toxicity. Examples: defatted powder of croton seed (Ba Dou Shuang, 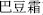 ), Kansui root (Gan Sui,
), Kansui root (Gan Sui, 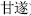 ) boiled with vinegar, Sichuan aconite root (Chuan Wu,
) boiled with vinegar, Sichuan aconite root (Chuan Wu, 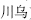 ) and wild aconite root (Cao Wu,
) and wild aconite root (Cao Wu, 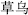 ) boiled for a long time, and Pinellia tuber (Ban Xia,
) boiled for a long time, and Pinellia tuber (Ban Xia, 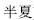 ) and Arisaema tuber (Nan Xing,
) and Arisaema tuber (Nan Xing, 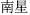 ) decocted with ginger and alum can all have toxicity reduced, as described.
) decocted with ginger and alum can all have toxicity reduced, as described.
(c)To change properties of herbs and expand their uses
Appropriate preparation can change cold or hot nature and augment effects of herbs. For example, dried Rehmannia root (Sheng Di Huang, 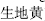 ), being cold in nature for removing heat from blood to stop bleeding, can be made into prepared Rehmannia root (Shu Di Huang,
), being cold in nature for removing heat from blood to stop bleeding, can be made into prepared Rehmannia root (Shu Di Huang, 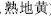 ) for warming and tonifying essence and blood. Prepared Arisaema (Zhi Nan Xing,
) for warming and tonifying essence and blood. Prepared Arisaema (Zhi Nan Xing,  ) being warm and dry in nature for resolving cold phlegm, expelling wind, and alleviating spasm, can be made into biled Arisaema (Dan Nan Xing,
) being warm and dry in nature for resolving cold phlegm, expelling wind, and alleviating spasm, can be made into biled Arisaema (Dan Nan Xing,  ) with a cool and moist nature for removing heat, resolving phlegm, expelling wind, and arresting convulsions. Fleece-flower root (Shou Wu,
) with a cool and moist nature for removing heat, resolving phlegm, expelling wind, and arresting convulsions. Fleece-flower root (Shou Wu, 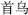 ), with its main effects of treating malaria and loosening the bowels, can be made into prepared fleece flower root (Zhi Shou Wu,
), with its main effects of treating malaria and loosening the bowels, can be made into prepared fleece flower root (Zhi Shou Wu, 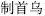 ) with its special effects of tonifying the liver and kidney and nourishing essence and blood. In addition, through preparation, herbs become easy to use and store. Also, the abnormal flavor and some unbeneficial ingredients are removed.
) with its special effects of tonifying the liver and kidney and nourishing essence and blood. In addition, through preparation, herbs become easy to use and store. Also, the abnormal flavor and some unbeneficial ingredients are removed.
(2) Methods of preparation
Methods for preparation of Chinese herbs include purification, preparation with water, preparation with fire, and preparation with both water and fire. They are closely related to their clinical usage.
(a)Stir-baking
Herbs are put into a pot over a fire, continually stir-baked to a certain extent, and taken out. According to the extent of heating, the herbs can be stir-baked yellow, stir-baked charred, or stir-baked carbonized. Being stir-baked yellow or stir-baked charred can moderate herbs’ properties or strengthen the effect of invigorating the spleen; and being stir-baked carbonized can strengthen the effects of stopping bleeding and arresting diarrhea.
(b)Stir-baking with auxiliary fluid
The common auxiliary fluids include wine, vinegar, honey, saline, and ginger juice. Herbs stir-baked with auxiliary fluid can strengthen effects, reduce toxicity, and remove abnormal flavor. Examples: Chinese Angelica root (Dang Gui, 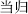 ) stir-baked with wine can strengthen the effects of promoting circulation of blood; Corydalis tuber (Yan Hu Suo,
) stir-baked with wine can strengthen the effects of promoting circulation of blood; Corydalis tuber (Yan Hu Suo, 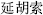 ) stir-baked with vinegar can strengthen its analgesic effect; and Kansui root (Gan Sui,
) stir-baked with vinegar can strengthen its analgesic effect; and Kansui root (Gan Sui, 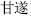 ) stir-baked with vinegar can reduce toxicity. In addition, herbs stir-baked with other auxiliary materials, including sand and talc powder, can make them crispy and enable their active ingredients to be easily decocted out, such as pangolin scales (Chuan Shan Jia,
) stir-baked with vinegar can reduce toxicity. In addition, herbs stir-baked with other auxiliary materials, including sand and talc powder, can make them crispy and enable their active ingredients to be easily decocted out, such as pangolin scales (Chuan Shan Jia,  ), stir-baked with sand.
), stir-baked with sand.
(c)Calcination
Herbs are directly or indirectly calcined over a fierce fire to make them crispy for easy crushing or carbonization. Most of the solid and hard mineral herbs or shells are directly calcined, such as dragon bone (Long Gu,  ) and oyster shell (Mu Li).
) and oyster shell (Mu Li).
(d)Roasting
Wrapped in moistened paper or flour paste, herbs are heated in smoldering cinders or roasted in an oven until the coating becomes charred to remove oil from the herbs orto moderate their properties — such as roasted Aucklandia root (Mu Xiang,  ) roasted ginger (Sheng Jiang,
) roasted ginger (Sheng Jiang,  ), and roasted nutmeg (Rou Dou Kou,
), and roasted nutmeg (Rou Dou Kou, 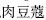 ).
).
(e)Steaming
Herbs are steamed solely or with auxiliary materials to change their properties, strengthen their potency, and reduce their toxic effects.
(f)Boiling
Herbs are boiled in water and auxiliary materials to reduce their toxicity, such as genkwa flower (Yuan Hua, 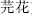 ) boiled with vinegar, and Sichuan aconite root (Chuang Wu,
) boiled with vinegar, and Sichuan aconite root (Chuang Wu, 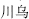 ) boiled with bean curd.
) boiled with bean curd.
(g) Water-refining
Mineral herbs insoluble in water are crushed, put in a mortar, ground with water into fine powder in suspension, then poured into a vessel for precipitation and dried — such as wet-refined cinnabar (Zhu Sha, 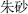 ) and water-refined talc (Hua Shi,
) and water-refined talc (Hua Shi, 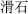 ).
).
In addition, there are fermentation, germination, frosting, and many other methods of preparation, such as medicated leaven, germinated barley (Mai Ya, 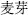 ), and defatted powder of croton seed (Ba Dou Shuang,
), and defatted powder of croton seed (Ba Dou Shuang, 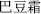 ).
).
Properties and Functions of Chinese Herbs
Chinese herbs have properties and functions that can be divided into four basic categories.
Four Properties and Five Flavors
The Four Properties (Si Qi, 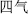 ) are cold, hot, cool, and warm. They are terms describing the effects, characteristics, and actions of the herbs. Herbs like gypsum (Shi Gao,
) are cold, hot, cool, and warm. They are terms describing the effects, characteristics, and actions of the herbs. Herbs like gypsum (Shi Gao, 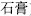 ), Anemarrhena rhizome (Zhi Mu,
), Anemarrhena rhizome (Zhi Mu, 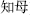 ), Coptis root (Huang Lian,
), Coptis root (Huang Lian, 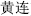 ), and Fresh Rehmannia root (Sheng Di Huang,
), and Fresh Rehmannia root (Sheng Di Huang, 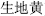 ), which have a cooling effect and relieve heat syndromes, are characterized as cool or cold. Herbs like Prepared aconite root (Fu Zi,
), which have a cooling effect and relieve heat syndromes, are characterized as cool or cold. Herbs like Prepared aconite root (Fu Zi, 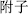 ), which relieve cold syndromes, are characterized as warm or hot. Herbs such as Poria (Fu Ling
), which relieve cold syndromes, are characterized as warm or hot. Herbs such as Poria (Fu Ling 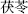 ), whose properties are neither cold nor hot, have neutral characteristics.
), whose properties are neither cold nor hot, have neutral characteristics.
The Five Flavors (Wu Wei, 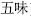 ) are pungent, sweet, sour, bitter, and salty. When the flavor is not obvious, it is known as bland. The flavors are terms that describe the therapeutic effects of herbs. Descurainia (Tingli Zi,
) are pungent, sweet, sour, bitter, and salty. When the flavor is not obvious, it is known as bland. The flavors are terms that describe the therapeutic effects of herbs. Descurainia (Tingli Zi, 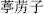 ) are Pungent herbs that disperse and promote the circulation of Qi and invigorate the blood. For instance, Ephedra (Ma Huang,
) are Pungent herbs that disperse and promote the circulation of Qi and invigorate the blood. For instance, Ephedra (Ma Huang, 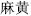 ) releases exterior syndromes by causing sweating; Costus root (Mu
) releases exterior syndromes by causing sweating; Costus root (Mu 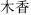 ) promotes the circulation of Qi; and Safflower (Hong Hua,
) promotes the circulation of Qi; and Safflower (Hong Hua, 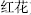 ) invigorates the blood.
) invigorates the blood.
Sweet herbs tonify, harmonize, and moderate. For example, Pilose asiabell root (Dang Shen, 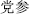 ) replenishes qi; Prepared Rehmannia root (Shu Di Huang,
) replenishes qi; Prepared Rehmannia root (Shu Di Huang, 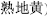 ) nourishes blood; and Licorice root (Gan Cao
) nourishes blood; and Licorice root (Gan Cao 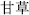 ) moderates and stops pain or harmonizes the actions of other herbs.
) moderates and stops pain or harmonizes the actions of other herbs.
Sour herbs absorb and control. For instance, Dogwood fruit (Shan Zhu Yu, 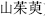 ) and Schisandra fruit (Wu Wei Zi,
) and Schisandra fruit (Wu Wei Zi, 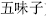 ) relieve seminal emissions and spontaneous sweating; and Chinese galla (Wu Bei Zi,
) relieve seminal emissions and spontaneous sweating; and Chinese galla (Wu Bei Zi, 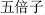 ) controls diarrhea. Also, some herbs are characterized as astringent. They have functions similar to those of sour herbs. For example, Dragon bone (Long Gu,
) controls diarrhea. Also, some herbs are characterized as astringent. They have functions similar to those of sour herbs. For example, Dragon bone (Long Gu, 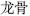 ) and Oyster shell (Mu Li,
) and Oyster shell (Mu Li, 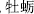 ) arrest spontaneous sweating; Red halloysite (Chi Shi Zhi,
) arrest spontaneous sweating; Red halloysite (Chi Shi Zhi, 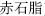 ) and Pomegranate rind (Shi Liu Pi,
) and Pomegranate rind (Shi Liu Pi, 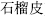 ) stop diarrhea; and Euryale seed (Qian Shi,
) stop diarrhea; and Euryale seed (Qian Shi, 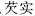 ) and Raspberry fruit (Fu Pan Zi,
) and Raspberry fruit (Fu Pan Zi, 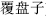 ) treat nocturnal emissions, frequent urination, and leukorrhea.
) treat nocturnal emissions, frequent urination, and leukorrhea.
Bitter herbs reduce and dry. For example, Rhubarb (Da Huang,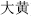 ) is used to move stools and reduce heat; Lepidium seed (Ting Li) reduces heat in the lungs and soothes asthma; Atractylodes rhizome (Cang Zhu,
) is used to move stools and reduce heat; Lepidium seed (Ting Li) reduces heat in the lungs and soothes asthma; Atractylodes rhizome (Cang Zhu, 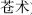 ) and Magnolia bark (Hou Po,
) and Magnolia bark (Hou Po, 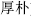 ) dry and transform turbid dampness; and Phellodendron bark (Huang Bai,
) dry and transform turbid dampness; and Phellodendron bark (Huang Bai, 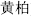 ) and Anemarrhena rhizome (Zhi Mu,
) and Anemarrhena rhizome (Zhi Mu, 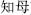 ) dry dampness and tonify Yin.
) dry dampness and tonify Yin.
Salty herbs soften hardness, release hardenings and nodules, and purge stools. For example, Glauber’s salt (Mang Xiao, 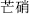 ) is used for constipation; and Ark shell (Wa Leng Zi,
) is used for constipation; and Ark shell (Wa Leng Zi, 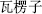 ) treats subcutaneous nodules and scrofula.
) treats subcutaneous nodules and scrofula.
Flavorless herbs transform dampness and promote urination. Poria (Fu Ling, 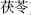 ) and Umbellate pore-fungus (Zhu Ling,
) and Umbellate pore-fungus (Zhu Ling, 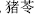 ) are classified as flavorless, and both benefit urination and drain dampness.
) are classified as flavorless, and both benefit urination and drain dampness.
When we describe the effects of herbs with the Four Properties and the Five Flavors, we can differentiate degrees of intensity. Herbs may be cold, slightly cold, or very cold; bitter, slightly bitter, or very bitter, etc. Some herbs, such as Schisandra fruit (Wu Wei Zi 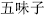 ), possess several flavors to summarize the multiple effects. In any event, every herb is cataloged as having a flavor and a property. These two characteristics are used to describe the complicated actions of the herb. Therefore, Ephedra (Ma Huang,
), possess several flavors to summarize the multiple effects. In any event, every herb is cataloged as having a flavor and a property. These two characteristics are used to describe the complicated actions of the herb. Therefore, Ephedra (Ma Huang, 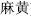 ) is a pungent and warm herb that disperses wind and cold; Lily bulb (Bai He,
) is a pungent and warm herb that disperses wind and cold; Lily bulb (Bai He, 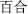 ) is sweet and cold and promotes the production of body fluids; and Astragalus root (Huang Qi,
) is sweet and cold and promotes the production of body fluids; and Astragalus root (Huang Qi, 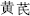 ) is sweet and warm and is used to replenish Qi.
) is sweet and warm and is used to replenish Qi.
Functional Tendencies
The functional tendencies of ascending, descending, floating, and sinking (Sheng Jiang Fu Chen, 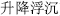 ) are a clinically useful categorization method. Herbs that ascend and float encourage upward and outward movement; they promote sweating, raise yang, and open the orifices of sense organs. Examples are Perilla leaf (Zi Su Ye,
) are a clinically useful categorization method. Herbs that ascend and float encourage upward and outward movement; they promote sweating, raise yang, and open the orifices of sense organs. Examples are Perilla leaf (Zi Su Ye, 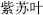 ), Bupleurum root (Chai Hu,
), Bupleurum root (Chai Hu, 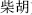 ), Cimicifuga rhizome (Sheng Ma,
), Cimicifuga rhizome (Sheng Ma, 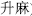 ), and Black false hellebore (Li Lu,
), and Black false hellebore (Li Lu,  ).
).
Herbs that descend and sink cause downward and inward movement, conduct Qi downward, promote urination and defecation, subdue yang, and calm the mind. Examples are Perilla seed (Su Zi,  ), Red ochre (Dai Zhe Shi,
), Red ochre (Dai Zhe Shi,  ), Rhubarb (Da Huang,
), Rhubarb (Da Huang,  ), and Cinnabar (Zhu Sha,
), and Cinnabar (Zhu Sha, 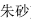 )
)
In general, the functional tendency of a herb is related to its flavor, property, and quality and processing. Herbs described as ascending and floating must be pungent or sweet in flavor as well as warm or hot in property, while herbs characterized as descending and sinking must be bitter, sour, or salty in flavor as well as cool or cold in property. The well-known TCM doctor Li Shizhen once described the relationships this way: “Sour or salty herbs have no function of ascending, pungent or sweet herbs have no function of descending, cold herbs have no function of floating and hot herbs have no function of sinking.”
Herb parts such as flowers and leaves that are light in quality usually have the functions of ascending and floating; herbs or substances that are heavy in quality, such as seeds, fruits, and minerals, have the functions of descending and sinking. In addition, processing and preparation may change the flavor and property of the herb and influence its functional tendencies. For example, frying herbs cause an ascending function; processing with ginger, a dispersing function; baking with vinegar, an astringing function; and preparing with salt, a downward function.
The combination of herbs is also a factor in determining the substance’s functional tendency and should be taken into consideration when formulating a herbal prescription. For example, Platycodon root (Jie Geng,  ) has a floating functional tendency, and Cyathula root (Niu Xi,
) has a floating functional tendency, and Cyathula root (Niu Xi, 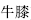 ) has a descending functional tendency. In combination, however, their functional tendencies will change.
) has a descending functional tendency. In combination, however, their functional tendencies will change.
Channel Tropism
A herb may selectively act on a particular part of the body to relieve pathogenic change in specific meridians and organs. The channel tropism (Gui Jing,  ) that a herb enters is determined by the symptoms it relieves. For example, Ephedra (Ma Huang,
) that a herb enters is determined by the symptoms it relieves. For example, Ephedra (Ma Huang, 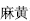 ) promotes sweating, soothes asthma, and benefits urination. It is indicated for fever, chills, and absence of sweating due to invasion by exogenous pathogenic wind and cold, dysuria, edema, and so on. Judged by the above indications and analyzed in accordance with the theories of the zang–fu organs and meridians, it can be determined that the herbs would enter the Lung and Urinary Bladder Meridians. Jujube (Da Zao,
) promotes sweating, soothes asthma, and benefits urination. It is indicated for fever, chills, and absence of sweating due to invasion by exogenous pathogenic wind and cold, dysuria, edema, and so on. Judged by the above indications and analyzed in accordance with the theories of the zang–fu organs and meridians, it can be determined that the herbs would enter the Lung and Urinary Bladder Meridians. Jujube (Da Zao, 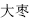 ) tonifies Qi in the spleen and stomach. It is indicated for poor appetite and loose stools due to weakness of the spleen and stomach. So we say that the herb enters the meridians of the spleen and stomach.
) tonifies Qi in the spleen and stomach. It is indicated for poor appetite and loose stools due to weakness of the spleen and stomach. So we say that the herb enters the meridians of the spleen and stomach.
The Four Properties, Five Flavors, and Channel Tropism are the approaches used to understand the actions of herbs. They are combined so as to relate to and supplement one another. Only by combining these approaches can a comprehensive prescription of herbs be made.
Toxicity
The words “toxic,” “non-toxic,” “very toxic,” and “slightly toxic” often appear in Chinese herbal medicine. The toxicity of herbs and substances can cause symptomatic reactions as well as have adverse effects on the body. No overdose of toxic herbs should be given, as this may lead to side effects. Non-toxic herbs are moderate in nature and, generally speaking, do not have obvious side effects. For example, Jujube (Da Zao,  ) and Poria (Fu Ling,
) and Poria (Fu Ling,  ) are non-toxic herbs, while aconite root (Fu Zi,
) are non-toxic herbs, while aconite root (Fu Zi,  ) and seed of nux-vomica poison nut (Ma Qian Zi,
) and seed of nux-vomica poison nut (Ma Qian Zi,  ) are toxic herbs.
) are toxic herbs.
Application of Chinese Herbs
Interaction of Herbs
Two or more herbs are combined to increase or promote their therapeutic effectiveness, to minimize toxicity or side effects, to accommodate complex clinical situations, and to alter their actions. Different combinations can cause variations in therapeutic effect. Traditionally, the results of combining herbs are classified as follows:
(1) Mutual reinforcement
Two or more herbs with similar properties are used in a combination to reinforce their therapeutic actions. For example, Rhubarb (Da Huang, 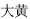 ) in combination with Glauber’s salt (Mang Xiao,
) in combination with Glauber’s salt (Mang Xiao, 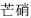 ) reinforces the function of purging downward; Gypsum (Shi Gao,
) reinforces the function of purging downward; Gypsum (Shi Gao, 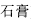 ) and Anemarrhena rhizome (Zhi Mu,
) and Anemarrhena rhizome (Zhi Mu, 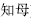 ) used together clear heat and subdue fire.
) used together clear heat and subdue fire.
(2) Mutual assistance
Multiple herbs are used in combination in which one is the principal herb and the others play a subsidiary role to enhance the therapeutic action. For example, Astragalus root (Huang Qi, 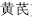 ) combined with Poria (Fu Ling,
) combined with Poria (Fu Ling, 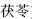 ) replenishes Qi, strengthens the spleen, and promotes urination; Gypsum (Shi Gao,
) replenishes Qi, strengthens the spleen, and promotes urination; Gypsum (Shi Gao, 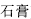 ) in combination with Cyathula root (Niu Xi,
) in combination with Cyathula root (Niu Xi, 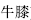 ) relieves toothache due to excess fire in the stomach.
) relieves toothache due to excess fire in the stomach.
(3) Mutual detoxification
This refers to the reduction in the toxicity or side effects of one herb by the addition of another. For example, adding Fresh ginger (Sheng Jiang, 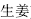 ) to Pinellia tuber (Ban Xia,
) to Pinellia tuber (Ban Xia, 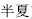 ) counteracts, or restrains, the latter’s toxicity.
) counteracts, or restrains, the latter’s toxicity.
(4) Mutual inhibition
In this combination of herbs, the property of one weakens or suppresses the action of the other. For example, Radish seed (Lai Fu Zi, 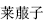 ) combined with Ginseng (Ren Shen,
) combined with Ginseng (Ren Shen, 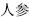 ) weakens the function of the latter in replenishing Qi.
) weakens the function of the latter in replenishing Qi.
(5) Mutual incapability
This refers to the ability of two herbs or substances to minimize or neutralize each other’s positive effects. Severe side effects may result when two incompatible herbs or substances are used in combination. Traditionally, there existed “18 incompatible medicinal herbs” and “19 mutually restraining medicinal herbs.” Among the 18 incompatible medicinal herbs, or substances, Tendrilled fritillary bulb (Chuan Bei Mu, 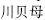 ), Pinellia tuber (Ban Xia,
), Pinellia tuber (Ban Xia, 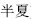 ), Bletilla tuber (Bai Ji,
), Bletilla tuber (Bai Ji, 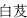 ), and Trichosanthes fruit (Gua Lou,
), and Trichosanthes fruit (Gua Lou, 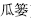 ) are incompatible with Sichuan aconite root (Wu Tou,
) are incompatible with Sichuan aconite root (Wu Tou, 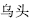 ); Asarum herb (Xi Xin,
); Asarum herb (Xi Xin, 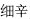 ), Peony (Shao Yao), White peony root (Bai Shao,
), Peony (Shao Yao), White peony root (Bai Shao, 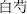 ), Ginseng (Ren Shen,
), Ginseng (Ren Shen, 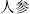 ), Glehnia root (Sha Shen,
), Glehnia root (Sha Shen, 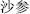 ), Salvia root (Dan Shen,
), Salvia root (Dan Shen, 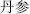 ), and Scrophularia (Xuan Shen,
), and Scrophularia (Xuan Shen, 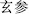 ) are incompatible with Black false hellebore (Li Lu,
) are incompatible with Black false hellebore (Li Lu, 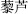 ); Peking spurge root (Da Ji,
); Peking spurge root (Da Ji, 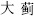 ) Genkwa flower (Yuan Hua,
) Genkwa flower (Yuan Hua, 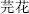 ), Kansui root (Gan Sui,
), Kansui root (Gan Sui, 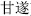 ), and Seaweed (Hai Zao,
), and Seaweed (Hai Zao, 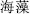 ) are incompatible with Licorice root (Gan Cao,
) are incompatible with Licorice root (Gan Cao, 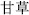 )
)
The 19 mutually restraining medicaments include Croton seed (Ba Dou, 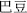 ), which restrains Pharbitis seed (Qian Niu Zi,
), which restrains Pharbitis seed (Qian Niu Zi, 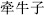 ); Cloves (Ding Xiang,
); Cloves (Ding Xiang, 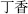 ), which restrains Curcuma root (Yu Jin,
), which restrains Curcuma root (Yu Jin, 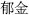 ); Ginseng bark (Ren Shen,
); Ginseng bark (Ren Shen, 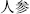 ), which restrains Trogopterus dung (Wu Ling Zhi,
), which restrains Trogopterus dung (Wu Ling Zhi, 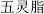 ); Cinnamon bark (Rou Gui,
); Cinnamon bark (Rou Gui, 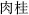 ) which restrains Red halloysite (Chi Shi Zhi,
) which restrains Red halloysite (Chi Shi Zhi, 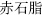 ); Sulfur (Liu Huang,
); Sulfur (Liu Huang, 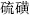 ), which restrains Mirabilite (Po Xiao,
), which restrains Mirabilite (Po Xiao, 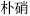 ) Mercury (Shui yin,
) Mercury (Shui yin, 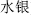 , which restrains Arsenic Trioxide (Pi Shuang,
, which restrains Arsenic Trioxide (Pi Shuang, 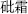 ); Lang Du root (Lang Du,
); Lang Du root (Lang Du, 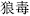 ), which restrains Litharge (Mi Tuo Seng,
), which restrains Litharge (Mi Tuo Seng, 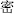
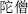 ), Monkshood root (Chuan Wu,
), Monkshood root (Chuan Wu,  ) and Wild aconite root (Cao Wu,
) and Wild aconite root (Cao Wu, 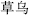 ), which restrain Rhinoceros horn (Xi Jiao,
), which restrain Rhinoceros horn (Xi Jiao, 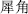 ); and Mirabilite (Po Xiao,
); and Mirabilite (Po Xiao, 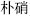 ) which restrains Burreed tuber (San Leng,
) which restrains Burreed tuber (San Leng, 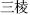 ).
).
Precautions and Contraindications
(1) Precautions and contraindications in combination
The historical medical literature contraindicates certain herbs and substances. These include the 18 incompatible medicinal herbs and the 19 mutually restraining medicinal herbs.
(2) Precautions and contraindications during pregnancy
It is contraindicated to prescribe herbs with strong actions or toxicity, especially Croton seed (Ba Dou, 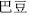 ), Pharbitis seed (Qian Niu Zi,
), Pharbitis seed (Qian Niu Zi, 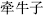 ), Peking spurge root (Da Ji, A
), Peking spurge root (Da Ji, A 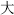
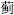 ) and Burreed tuber (San Leng,
) and Burreed tuber (San Leng, 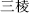 ), for pregnant women. Pungent and hot herbs that promote circulation of Qi and remove stagnation of Qi and blood should be used with caution during pregnancy. They include Peach seed (Tao Ren,
), for pregnant women. Pungent and hot herbs that promote circulation of Qi and remove stagnation of Qi and blood should be used with caution during pregnancy. They include Peach seed (Tao Ren, 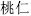 ), Safflower (Hong Hua,
), Safflower (Hong Hua, 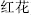 ) Rhubarb (Da Huang,
) Rhubarb (Da Huang, 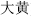 ), and Prepared aconite root (Fu Zi,
), and Prepared aconite root (Fu Zi, 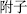 ).
).
(3) Precautions and contraindications in food intake
Certain foods may influence the action of herbs or bring about some abnormalities. It is advisable, in general, not to eat raw, cold, greasy, strong-smelling, or spicy food while taking medicine. The historical medical literature records that Dichroa root (Chang Shan, 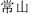 ) is contraindicated with onion; Rehmannia root (Di Huang,
) is contraindicated with onion; Rehmannia root (Di Huang, 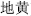 ) and Fleeceflower root (He Shou Wu,
) and Fleeceflower root (He Shou Wu, 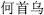 ) are contraindicated with onion, garlic, and turnip; Mentha (Bo He,
) are contraindicated with onion, garlic, and turnip; Mentha (Bo He, 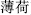 ) is contraindicated with turtle meat; Poria (Fu Ling,
) is contraindicated with turtle meat; Poria (Fu Ling, 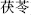 ) is contraindicated with vinegar; and Turtle shell (Bie Jia,
) is contraindicated with vinegar; and Turtle shell (Bie Jia, 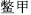 ) is contraindicated with three-colored amaranth.
) is contraindicated with three-colored amaranth.
Each herb has its own particular indications. The clinician should never select herbs at random. He or she must know the properties, flavors, and actions of the herbs. For example, Ephedra (Ma Huang, MM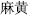 ) is pungent and warm in flavor and property and promotes sweating. It is used to treat fever, chills, and absence of sweating due to an invasion of wind and cold. It is contraindicated in deficiency exterior syndrome with the symptoms mentioned above.
) is pungent and warm in flavor and property and promotes sweating. It is used to treat fever, chills, and absence of sweating due to an invasion of wind and cold. It is contraindicated in deficiency exterior syndrome with the symptoms mentioned above.
Principle of Chinese Herbal Formulation
The Chinese Herbal Prescriptions presented in Chapter 20 illustrate the practical application of the theories of Chinese Medicine in general and Chinese Herbs in particular. As with the individual herbs, the prescriptions are grouped by their main functions.
Studying the prescriptions put forward in this chapter will yield a better understanding of the theories of Chinese Medicine and how to apply them in terms of mapping a treatment strategy and identifying appropriate herbal prescriptions for various diseases. The eight treatment strategies in Traditional Chinese Medicine are dispersing, sweating, warming, heat-clearing, purgation, vomiting, harmonizing, and tonifying.
Although each section of the chapter starts with individual representative herbs, it is important to understand that, in practice, it is the herbal combination that is used to effect the changes needed to correct health imbalances. The classical Chinese herbal prescriptions included in this book are excellent examples proving that appropriate multiple herbs not only enhance the overall therapeutic effect but broaden it as well. It is possible to individualize the treatment, matching the formula in as much detail as possible to the nuances of the patient’s syndrome. Finally, these classical prescriptions comprise well-balanced and harmonious herbal combinations that reduce the risk of side effects posed by the use of individual herbs. Thus, through their mutual restraint or mutual reinforcement, herbs can fully display their actions while limiting potential toxic side effects. Indeed, modern scientific research in China and other parts of the world upholds the classical application of multiple herbs in combination as a sound and powerful practice.
Additionally, part of the power and utility of Chinese Herbal Prescriptions is the flexibility to alter the prescription to fit the individual case. Ways to do so include substituting alternate component herbs, changing the dosage, and modifying the dosage form (decoction, powder, pill, etc.).
To Elaborate on the Concepts Touched on Under “Interaction of Herbs” (above), the Components of a Formula and Their Roles are:
(1)Chief (or monarch): The principal herb; the essential ingredient aiming at the syndrome.
(2)Assistant (minister): Strengthens the effect of the monarch.
(3)Adjuvant: Treats accompanying syndromes; reduces side effects of the monarch; provides a supplementing effect.
(4)Guide: Leads the formula to the affected area; regulates the properties of the other composition.
As mentioned, the herbal prescriptions presented here are classical ones, some going back 2000 years. Thus, the herbs are listed in their traditional order, which may not strictly follow the format of monarch, minister, adjuvant, and guide. In the long and constantly evolving history of traditional Chinese medicine, these terms are relatively new and did not exist at the time these formulas were devised and perfected. However, the role of each herb is clearly delineated in the discussion.
The Following Organization is Adhered to Throughout the Chapter in Order to Facilitate Reference:
(1)Composition: Each formula begins with a list of herbs, which includes the component herbs, their common names and Chinese pinyin names, as well as the required quantity of each herb.
(2)Preparation: A brief description of how the formula is prepared, including any alternate methods, is listed under “Administration.”
(3)Functions: The Functions which each herbal formula performs are then listed.
(4)Indications: The “Indications” section defines the conditions, including manifestations, in terms of the language of traditional Chinese medicine for which the herbal formula is applicable.
(5)Formula Analysis: An explanation of how the condition affects the patient’s Qi, meridians and collaterals, blood, body fluids, etc. and the strategy by which to overcome the condition are presented, along with the component herbs and the roles they play in creating the overall effect of the formula.
(6)Clinical Applications in Bio-Medicine: This section uses bio-medical terminology to identify specific maladies against which the formula has proven effective.
(7)Modifications: Adjustments to the formula occasioned by special symptoms are presented.
(8)Cautions: The “Cautions” section details any additional advice, including contraindications, that is necessary for effecting a positive treatment outcome.

